LESSON 7 Remove an Airway Obstruction in a Child or Infant.
TEXT ASSIGNMENT Paragraphs 7-1 through 7-4.
LESSON OBJECTIVES After completing this lesson, you should be able to:
7-1. Identify the proper procedures for removing an airway obstruction in a conscious child.
7-2. Identify the proper procedures for removing an airway obstruction in an unconscious child.
7-3. Identify the proper procedures for removing an airway obstruction in a conscious an infant.
7-4. Identify the proper procedures for removing an airway obstruction in an unconscious infant.
SUGGESTION After you have completed the text assignment, work the exercises at the end of this lesson before beginning the examination. These exercises will help you to achieve the lesson objectives.
Overview
7-1. REMOVE UPPER AIRWAY OBSTRUCTION IN A CONSCIOUS CHILD
a. Good Air Exchange. If the child is coughing, encourage him to continue coughing as long as he is coughing with enough force to expel the object.
b. Poor Air Exchange or Complete Blockage. If the child’s coughs are weak or nonexistent or if he has difficulty breathing accompanied by a harsh, high pitched noise when inhaling (stridor), administer abdominal thrusts to expel the obstruction. As you prepare to administer the thrusts, call for help, but do not delay performing the thrusts to seek help.
(1) If the child is sitting or standing, perform abdominal thrusts using the same procedures as for an adult (paragraph 5-5). Continue administering thrusts until the obstruction is expelled or until the child loses consciousness. If the child loses consciousness, lower the child to the ground and administer modified abdominal thrusts as described in paragraph 7-2.
(2) If the child is choking with poor or no air exchange and is lying down, position the child flat on his back on a firm surface and administer modified abdominal thrusts as described in paragraph 7-2.
7-2. REMOVE UPPER AIRWAY OBSTRUCTION IN AN UNCONSCIOUS CHILD
The steps given below assume the child is conscious and lying down [paragraph 7-1b(2)] or lost consciousness while you were administering abdominal thrusts [paragraph 7-1b(1)]. If you discovered an airway obstruction while performing rescue breathing [paragraph 6-4c(2)], you will have already performed the steps given in paragraphs a through c below.
a. Call for help if you have not done so or if help has not arrived.
b. Lay the child on his back on a firm, flat surface, open his airway, and check for breathing (paragraph 6-2).
c. If the child is not breathing, attempt to administer two ventilations (paragraph 6-3). If the airway is blocked, reposition the head and attempt to administer two ventilations again.
d. If the airway is still blocked, administer modified abdominal thrusts to expel the object.
NOTE: Abdominal thrusts are preferred for clearing the airway of a child. If abdominal thrusts cannot be administered due to abdominal injuries, perform chest thrusts by locating the compression site (paragraph 4-1d) and administering thrusts with the heel of one hand sufficient to depress the lower half of the sternum 1 to 1 1/2 inches. Make each thrust separate and distinct.
(1) Abdominal thrust–large child. If the child is large, administer abdominal thrusts using the same procedures as for an adult [paragraph 5-6f(1)].
(2) Abdominal thrust–small child.
(a) If the child is small, position yourself at the child’s side. Striding the casualty’s thighs is not recommended for small children. If the child is on a table, you may prefer to stand at his feet and deliver the thrusts.
(b) Place the heel of your hand that is closest to the child’s feet on his abdomen. The heel should be on the midline slightly above the navel and well below the rib cage and xiphoid process. Turn your hand so your fingers are straight out and pointing toward the child’s head.
(c) Place the heel of your hand on top of the first hand.
(d) Administer quick, but gentle, inward and upward thrusts.
e. If the obstruction has not been expelled after five thrusts, open his mouth using jaw-tongue lift [paragraph 5-6c(3)] and look for the obstruction. If you see the obstruction, perform a finger sweep [paragraphs 5-6c(5), (6), and (7)] and remove the obstruction. Do not perform a blind finger sweep since you may push the obstruction deeper into the child’s throat.
f. Attempt to administer two ventilations again (paragraph 6-3). If the airway is still blocked, perform up to five abdominal thrusts and visually check for the obstruction again. Once the obstruction is removed, perform rescue breathing or CPR (Lesson 6) as needed if the child does not begin breathing again on his own.
7-3. REMOVE UPPER AIRWAY OBSTRUCTION IN A CONSCIOUS INFANT
If a head or spinal injury is suspected, place the infant on a firm surface and administer chest thrusts and finger sweeps (no backblows) as needed. If a head or spinal injury is not suspected (for example, the infant is choking on something he just swallowed), use the procedures given below to remove the obstruction. The rescuer should be in a kneeling or sitting position. (Note that backblows are administered to infants, but not to children or adults.)
a. Call for Help. Call for help, but do not leave the casualty or delay administering chest thrusts in order to seek help. You may need someone to take you and the infant to a medical facility while you continue to perform lifesaving measures.
b. Position Infant for Backblows.
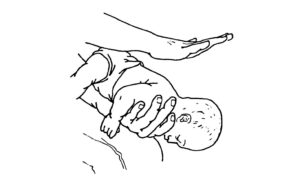
(1) Small infant. Roll the infant’s body lengthwise over your arm so the infant is straddling your forearm with his rear toward you and his back up as shown in figure 7-1. Support the infant’s head with the thumb and fingers of your hand. Rest your forearm on your thigh to provide support. Be sure the infant’s head is lower than the trunk of his body.
(2) Large infant. If the infant is too large to straddle your arm, lay the casualty’s body across your thighs with his head lower than the trunk of his body. Position the arm that will not be used to administer backblows under the infant’s body so that the hand supports the infant’s head and neck. The forearm under the infant’s chest will provide a firm surface for the backblows.
c. Administer Backblows. Administer five glancing backblows (figure 7-1). A backblow is administered by striking the infant on the spine between his shoulder blades with the heel of your free hand. The five blows should be delivered within 5 seconds.
d. Position Infant for Chest Thrusts. Chest thrusts are used instead of abdominal thrust because the force of abdominal thrusts could injury the abdominal organs of an infant.
(1) Small infant. Place your free arm over the infant’s back with your arm over his spine and your hand resting on the back of his head. Turn the infant over so he is now positioned with his face up and you are supporting the back of his head in the palm of your hand. Rest your forearm on your thigh. Make sure the infant’s head is lower than his trunk. The forearm under the infant’s back will provide the firm surface needed for the chest thrusts.
(2) Large infant. If the infant is too large to straddle your arm, turn the infant over and lay his body across your thighs with his head lower than the trunk of his body. Put your arm (the arm not being used to deliver chest thrusts) under the infant’s head and neck. The forearm under the infant’s back will provide a firm surface for the chest thrusts.
e. Administer Chest Thrusts. Chest thrusts are used rather than abdominal thrusts due to the danger of injury to abdominal organs from abdominal thrusts. The chest thrusts are performed in the same manner as are CPR chest compressions for infants (paragraph 6-6) except the thrusts are delivered at a somewhat slower rate.
(1) Draw an imaginary line on the casualty’s chest connecting his nipples.
(2) Place the index finger of your free hand just under the imaginary line on top of the infant’s sternum.
(3) Place your middle and ring fingers on the sternum so that they are below (closer to the infant’s feet than) your index finger.
(4) Lift your index finger from the infant’s sternum.
(5) Press straight down with the tips of the middle and ring fingers so the sternum is depressed 1/2 to 1 inch.
(6) Relax pressure without removing your fingertips from the compression site and allow the sternum to return to its normal position.
(7) Repeat the chest thrusts until a total of five chest thrusts have been administered or the object has been expelled.
f. Repeat Backblows and Chest Thrusts. Repeat the series of five backblows and five chest thrusts until the obstruction is expelled or until the infant looses consciousness.
(1) If the obstruction is expelled, check the infant for breathing. Administer rescue breathing or CPR (lesson 6) as needed if the infant does not resume breathing on his own.
(2) If the infant loses consciousness, use the procedures given in paragraph 7-4.
7-4. REMOVE UPPER AIRWAY OBSTRUCTION IN AN UNCONSCIOUS INFANT
The steps given below assume the infant lost consciousness while you were administering rescue thrusts [paragraph 7-3f(2)] or you discovered an airway obstruction while performing rescue breathing [paragraph 6-4c(2)]. If a head or spinal injury is suspected, administer chest thrusts and finger sweeps, but do not administer backblows. The procedures given in the following paragraphs assume that no head or spinal injury is present.
a. Call for Help. Call for help if you have not done so and determine unresponsiveness.
b. Position Infant for Foreign Body Check.
(1) Small infant. Turn the infant face up with your arm under the infant’s back so your hand is supporting the back of his head and your forearm is under his spine. Rest your forearm on your thigh so the infant’s head is lower than his trunk.
(2) Large infant. If the infant is too large to straddle your arm, lay the casualty’s body across your thighs with his face up and his head lower than the trunk of his body. Position the arm that will not be used to remove the object under the infant’s body with the hand supporting the infant’s head and neck.
c. Open the Infant’s Mouth. Open the infant’s mouth using a tongue-jaw lift technique.
(1) Place the thumb of one hand (the hand not supporting his head) into his mouth and over his tongue.
(2) Wrap the fingers of the hand around his lower jaw.
(3) Lift the jaw and tongue forward.
d. Remove Any Visible Foreign Matter. If you see any foreign matter in the infant’s mouth or throat, remove the obstruction with a finger sweep (paragraph 5-6c). Do not perform a blind finger sweep since this action could force the obstruction deeper into the infant’s throat.
e. Check for Breathing. Tilt the infant’s head back slightly and lift the infant’s chin to open the airway. Look, listen, and feel for signs of breathing (chest or abdomen rising and falling, sounds of breathing, exhaled air blowing on cheek).
(1) If spontaneous breathing occurs, maintain the airway and check for other injuries.
(2) If spontaneous breathing does not occur, attempt to administer ventilations.
f. Administer Two Ventilations. If the infant is not breathing on his own, administer two ventilations using the mouth-to-mouth-and-nose method. Even if the obstruction has not been removed, your efforts may have caused it to shift enough so rescue breathing can now be administered.
(1) Maintain the airway by lifting the infant’s chin with the free hand. Do not hyperextend the neck.
(2) Take a breath. (Do not take a deep breath since you will not need to blow much air into the infant’s smaller lungs.)
(3) Place your mouth over the infant’s mouth and nose. Make sure that your mouth forms an airtight seal so that air will not escape when you blow air into his mouth and nose.
(4) Blow a small puff of air (only enough to make the chest rise) into the infant’s mouth and nose. Observe the chest out of the corner of your eye as you administer the breath.
(5) After blowing into the infant’s mouth and nose, break the seal over his face and allow air to escape. His chest should fall somewhat as air escapes after you break the seal. You may be able to hear or feel the exhaled breath.
(6) Take another breath, seal your mouth over the infant’s mouth and nose again, and administer a second puff of air. It should take 3 to 5 seconds to administer both breaths.
g. Evaluate Your Efforts.
(1) If your ventilations were successful (chest rose and fell), check the infant’s pulse (paragraph 6-5).
(a) If the pulse is absent, administer CPR (paragraph 6-6).
(b) If a pulse is present, administer ventilations at the rate of one ventilation every 3 seconds (20 ventilations per minute). Check the pulse again every few minutes. Also check for spontaneous breathing when you check the pulse. If the pulse is absent, administer CPR.
(c) Continue your efforts until the infant is breathing spontaneously or until you are relieved by a physician or other medical authority. If possible, evacuate the casualty to a medical treatment facility as you perform rescue breathing/CPR.
(2) If your ventilations were not successful (air did not go in and the chest did not rise), perform backblows (if no spinal or head injury), chest thrusts, finger sweeps (when appropriate), and ventilations as given in the following paragraphs until the obstruction is removed.
h. Call for Help. Call for help again. If a second rescuer is available, have him seek medical assistance.
i. Position Infant for Backblows. Position the infant for backblows using the procedures given in paragraph 7-3b(1) if the casualty is a small infant and in paragraph 7-3b(2) if the casualty is a large infant.
j. Administer Backblows. Administer five backblows by striking the infant on the spine between his shoulder blades with the heel of your free hand. The five blows should be delivered within 3 to 5 seconds.
k. Position Infant for Chest Thrusts. Position the infant for chest thrusts using the procedures given in paragraph 7-3d(1) if the casualty is a small infant and in paragraph 7-3d(2) if the casualty is a large infant.
l. Administer Chest Thrusts. Perform chest thrusts in the manner described in paragraph 7-3e. Continue until the obstruction has been expelled or until you have administered five chest thrusts.
m. Continue Efforts to Expel Obstruction. If the chest thrusts did not expel the object, continue your efforts until the object is expelled or you are ordered to stop by a medical authority. If possible, evacuate the casualty as you continue your efforts.
(1) Open the infant’s mouth using a tongue-jaw lift technique and remove any visible foreign matter with a finger sweep.
(2) Open the infant’s airway and check for signs of breathing. If spontaneous breathing occurs, maintain the airway.
(3) If the infant does not resume breathing on his own, administer two ventilations using the mouth-to-mouth-and-nose method.
(a) If your ventilations were successful, check the infant’s pulse. If a pulse is absent, administer CPR (paragraph 6-6). If a pulse is present, administer rescue breathing at the rate of one ventilation every 3 seconds and recheck the pulse again every few minutes.
(b) If your ventilations were not successful (air did not go in and chest did not rise), continue with your efforts to expel the obstruction.
(4) If your ventilations were not successful, position the infant for backblows and administer five back blows.
(5) If the backblows did not expel the obstruction, position the infant for chest thrusts and administer five chest thrusts.
(6) If the chest thrusts did not expel the obstruction, continue with your efforts to expel the obstruction [paragraph 7-4m(1) through (6)].
NOTE: Public education is vital to alleviate fear of risk of disease transmission during CPR. Use barriers as recommended by the Centers for Disease Control and the Occupational Safety and Health Administration.
